COVID-19
Herd Immunity Re-Revisited
4. Incomplete immunity
Coronaviruses differ from other RNA viruses that they have a proof-reading RNA polymerase that minimizes mutations. This implies that coronaviruses have different strategies to escape immune responses.
- They limit the induction of antivirus immunity by the undermining interferon responses.
- They overstimulate the immune system by superantigen activities to abrogate immune responses before these mature.
- They, like other airway viruses they avoid virus neutralization by not having an early passage through peripheral blood.
4.1 Vaccination
Being vaccinated and receiving booster vaccination is much safer for everyone than being infected. Vaccination may offer considerable protection from severe disease, but this still is incomplete. Omicron is not a mild disease and yields a high mortality, even though the infection-fatality ratio (IFR) is clearly less than with the Delta variant.
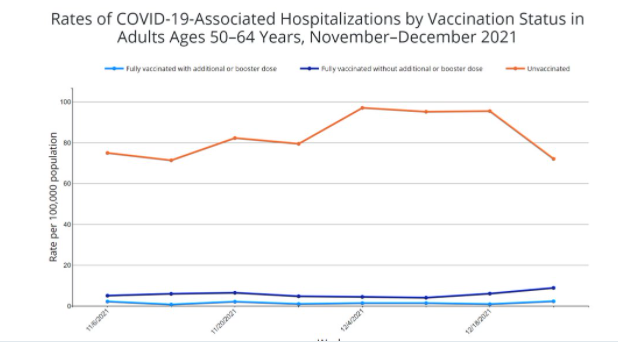
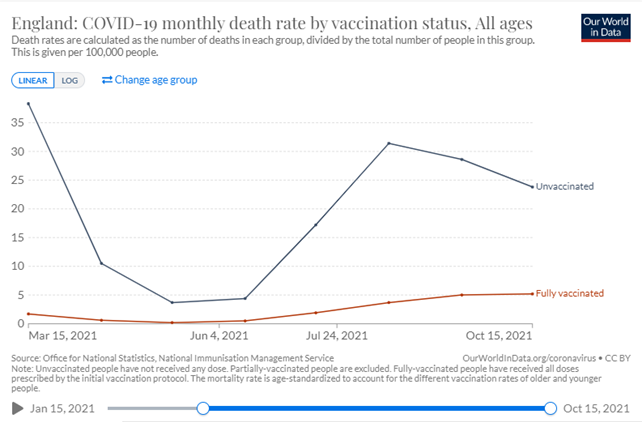
Vaccination protects from hospitalizations, but previous infections protect only very limited from reinfections and hospitalizations in the longer term (Figure 12). This illustrates that infection-induced immunity is a poor strategy. The absolute effect of protecting from mortality varies with the incidence of COVID-19 fatalities (Figure 13). The consistent lower line of the vaccinated population illustrates that vaccination holds no major risks.
Vaccination protects from hospitalizations, but previous infections protect only very limited from reinfections and hospitalizations in the longer term (Figure 12). This illustrates that infection-induced immunity is a poor strategy. The absolute effect of protecting from mortality varies with the incidence of COVID-19 fatalities (Figure 13). The consistent lower line of the vaccinated population illustrates that vaccination holds no major risks.
Figure 12. Hospitalization per vaccination status.
Figure 13. Vaccination protects against lethal disease, this is most visible when infections are high.
4.2 Immune uncertainty
Statistical data often show that vaccinations and boosters protect the population on average. It is unarguably shown that protection against infection is best early after vaccination, and superior to the risk reduction by a previous infection. Individual protection differs strongly between people. In the complexity of immune factors, it is not clear which factors contribute how much to protection. Neutralizing antibodies are likely to present some part of immune protection and can be measured easily.
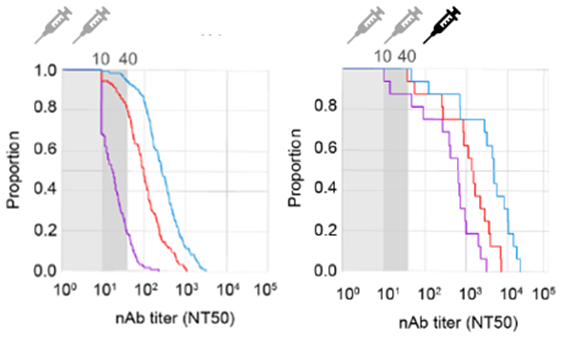
Booster vaccinations will increase neutralizing antibody responses on average but not everyone is fully protected (Figure 14). Immunity has a large heterogeneity in the population, so people may still become (seriously) ill or develop long covid after mild disease. In recently boosted people, Omicron might be less severe.
It should be noted that being protected now is no guarantee for long-term protection. Immunity against coronaviruses tends to wane more rapid than against other diseases. Just like the common cold coronaviruses, some people will fall ill to the SARS-2 multiple times per year, others rarely, like only in stressful periods in their lives.
Booster vaccinations will increase neutralizing antibody responses on average but not everyone is fully protected (Figure 14). Immunity has a large heterogeneity in the population, so people may still become (seriously) ill or develop long covid after mild disease. In recently boosted people, Omicron might be less severe.
It should be noted that being protected now is no guarantee for long-term protection. Immunity against coronaviruses tends to wane more rapid than against other diseases. Just like the common cold coronaviruses, some people will fall ill to the SARS-2 multiple times per year, others rarely, like only in stressful periods in their lives.
Figure 14. Heterogeneity in neutralizing antibodies after vaccination (left) or boosting (right) against Wild type virus (blue), Delta (red) or Omicron (purple). Shades of grey are insufficiently or unprotected people.
4.3 Reinfections
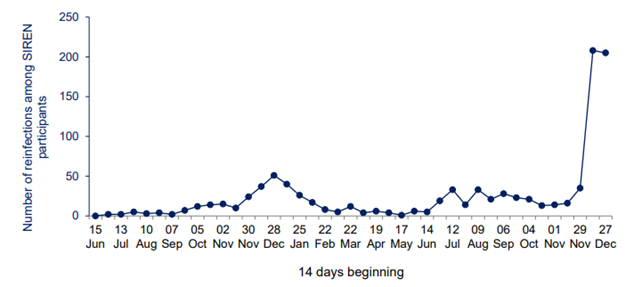
The idea behind herd immunity is that people are protected against reinfection during a very long time. Reinfections illustrate that no herd immunity is built for coronaviruses. Numerous reports show that people who had a SARS-2 infection can be followed by reinfection. A small systematic review with control for reinfection showed that nearly 13% had less, 69% had similar and 19% had worse symptoms in the second episode. The reinfections occurred often in young people and on average 3 months (3 weeks to 5 months) after the first infection (Figure 15).
Coronaviruses evolve to keep infecting people which results in people being infected multiple times, and repeated risks of long covid and severe disease. Immunity after SARS-2 infection wanes quickly, and re-infections will occur. Increasing virus circulation causes people to become infected more often, although vulnerable people might choose to protect themselves. Hospitalization levels in children have risen in the Omicron wave due to this strategy.
Coronaviruses evolve to keep infecting people which results in people being infected multiple times, and repeated risks of long covid and severe disease. Immunity after SARS-2 infection wanes quickly, and re-infections will occur. Increasing virus circulation causes people to become infected more often, although vulnerable people might choose to protect themselves. Hospitalization levels in children have risen in the Omicron wave due to this strategy.
Figure 15. The number of reinfections.
4.4 Immune escape
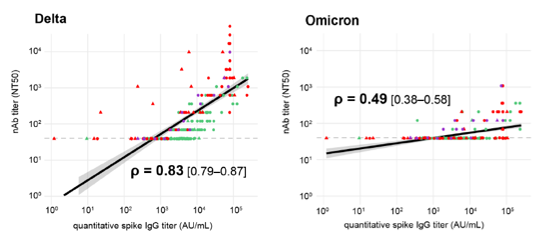
Omicron is not only better at escaping immune responses than Delta, it also is better in preventing effective immune responses. Immune responses after Omicron yield only few neutralizing antibodies, raising doubt if it would protect against other variants (Figure 16).
Figure 16. All versus neutralizing antibodies against and after Delta & Omicron breakthrough infections. Breakthrough infections of Delta (red) and Omicron (purple) and uninfected vaccinated (green).
John. J.L. Jacobs. 18.02.2022